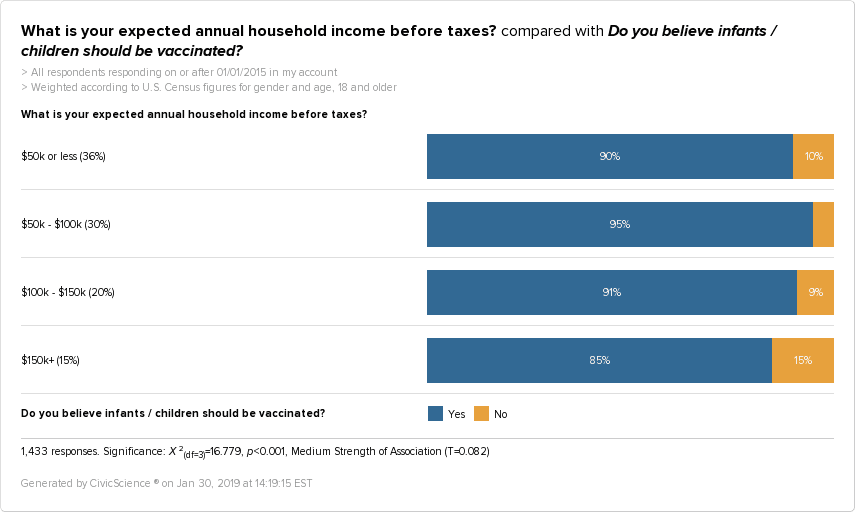The new year’s not off to a great start, with dangerous temperatures and a measles outbreak in Washington state that led to a state of emergency.
That coincides with the World Health Organization’s list of the top ten threats to global health in 2019, where “vaccine hesitancy” — “the reluctance or refusal to vaccinate despite the availability of vaccines” — ranks right up there alongside climate change and Ebola.
Unpacking that, according to the WHO, there isn’t a sole reason why some don’t get vaccinated or don’t vaccinate their children. Rather, there are several. Financial concerns and access to healthcare can play roles, as can feelings of complacency, lack of confidence in vaccines, and religious and personal beliefs.
Here in the U.S., some are attributing the recent Washington outbreak to an anti-vax population in that region (and allowances by state legislation). One of the most popularized deterrents for childhood vaccination has been fear over an unsubstantiated link between the MMR vaccine (measles, mumps, and rubella) and autism in children.
That leaves most of us wondering where Americans really stand not just on MMR vaccination, but on vaccination across the board, and what it all means going forward.
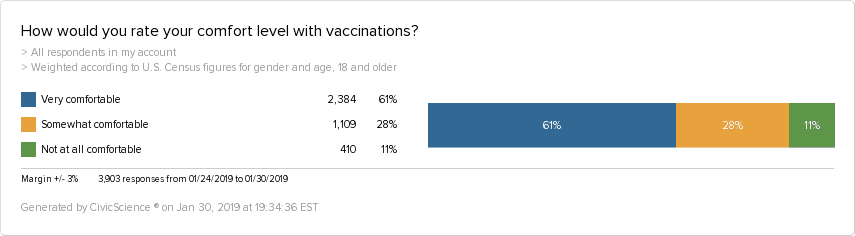
In a series of recent online polls of 1,700 to 3,000-plus respondents, CivicScience prodded the public on their feelings about vaccines. When it comes to general attitudes, most U.S. adults surveyed feel some level of comfort with vaccinations, while 11% don’t feel comfortable at all.
Do people have different feelings towards different vaccinations? Yes, it turns out. While half of respondents support both mandatory vaccinations required for school attendance unless exempt (e.g., tetanus, MMR) and elective vaccinations (e.g., flu shot, shingles), a little over one-third only support mandatory vaccinations, while the remaining population is split evenly between supporting elective vaccinations exclusively or no vaccinations at all.
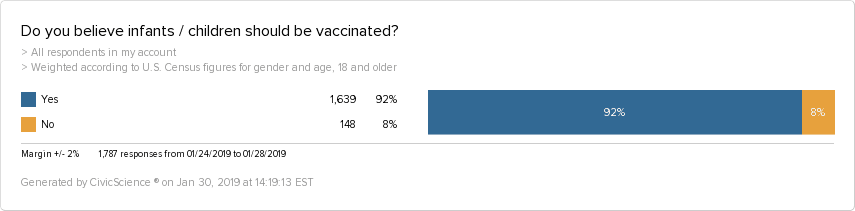
Honing in on the measles outbreak and opinions on infant and child vaccinations under which the MMR vaccine falls, the majority of U.S. adults believe children should be vaccinated, while 8% do not.
Eight percent seems small, but the recent measles outbreak indicates it’s obviously not insignificant. Consider that in light of an upsurge in measles cases in the past few years in certain regions, including North America and Europe.
While measles was declared eliminated in the U.S. in 2000, even though small outbreaks have consistently occurred since, the fear is that a growth in numbers of unvaccinated children threaten “herd immunity” — the percentage of the population that needs to be vaccinated in order to stop the spread of a disease. With measles, that’s said to be 92-95%.
Who exactly is for and against childhood vaccination and what can be learned from them?
Young Adults are Less In Favor
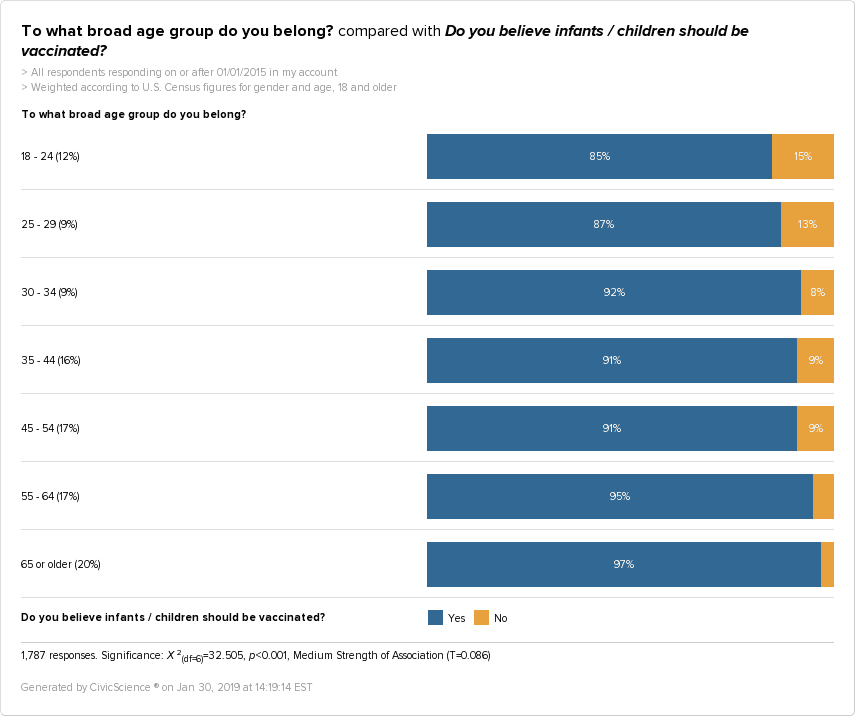
Age appears to play a key role. The survey shows that young U.S. adults up to age 29 were significantly more likely to be against childhood vaccination, accounting for 15% of 18-24-year-olds. That’s nearly twice as high as 30 to 54-year-olds and three times or more higher than those 55 and older.
Those findings are in line with a report released last year by the European Commission, which found that younger EU adults had less confidence in the importance of MMR vaccines than older cohorts.
Interestingly, the survey revealed that when asked about vaccine comfort levels (as mentioned previously), young adults were not less comfortable with vaccines than older adults. It’s the question of childhood vaccination that’s most divisive.
Parental Status
Perhaps surprisingly, being a parent does not correlate with opinions on childhood vaccination. Childless folks are as likely to support childhood vaccinations as parents.
Education and Income
Is there a correlation between education level, income level, and feelings on childhood vaccines?
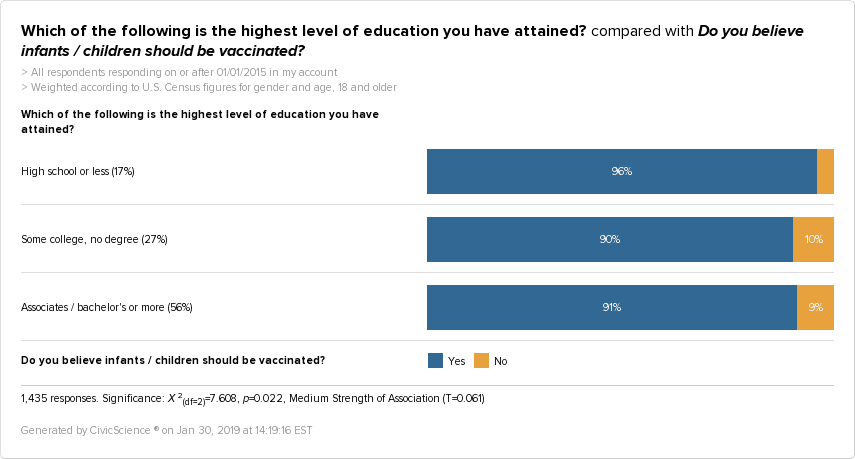
Yes, and it’s probably not what you were expecting. The survey revealed that adults with some college education and those with a degree(s) were more likely than those with a high school degree or less to be against the vaccination of infants and children.
And then there’s this. Solid middle-class earners ($50-100k per year) were the most favorable to childhood vaccination, while the highest earners in the survey ($150k+) were the least favorable.
While access to healthcare and financial issues have been found to play a role in vaccine hesitancy (which could be represented within the 10% of $50k and under earners), that doesn’t explain why those making income above the national average would be the most averse to childhood vaccination.
The survey also showed that childhood vaccination is slightly less favored by women than men and by city dwellers than suburban dwellers.
Personal Beliefs
Last but certainly not least, respondents varied on the question of childhood vaccination and personal beliefs.
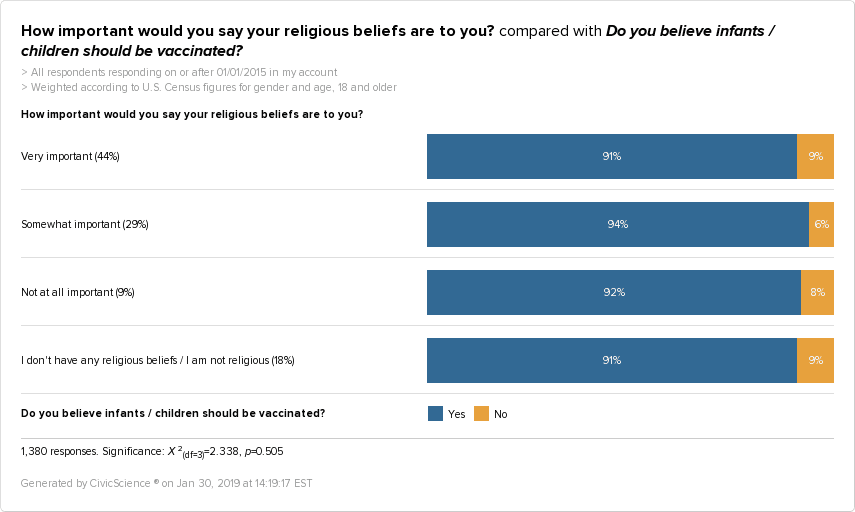
Religious Belief — Those unfavorable to childhood vaccination aren’t any more or less religious than other people:
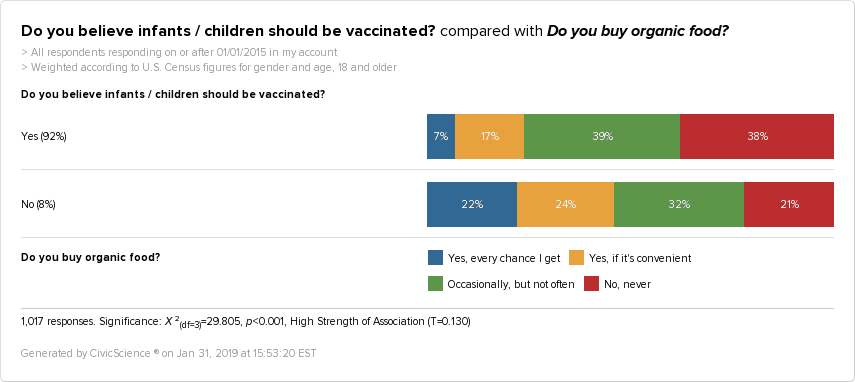
‘Natural’ Lifestyle — There is a huge correlation between those who don’t support childhood vaccination and organic food-buying. They are more than three times as likely to buy organic food regularly compared to adults who support childhood vaccination.
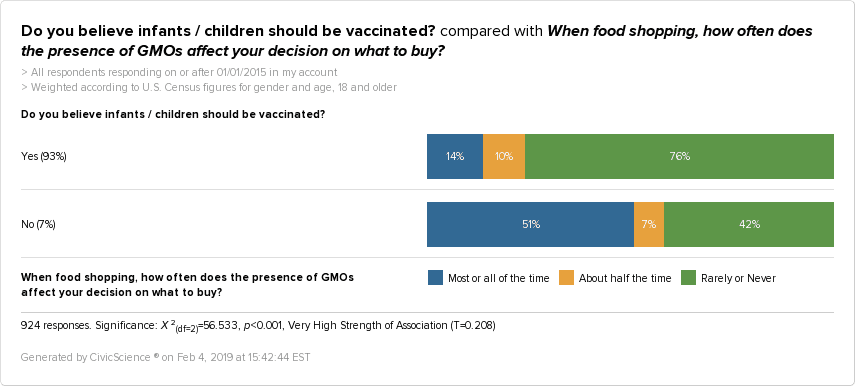
Also, they are 72% more likely to always be concerned with the presence of GMOs when shopping for food:
These findings are in line with research that suggests online anti-vaccination activists promote so-called “natural,” alternative lifestyles, opposed to the “artificial” practice of vaccination.
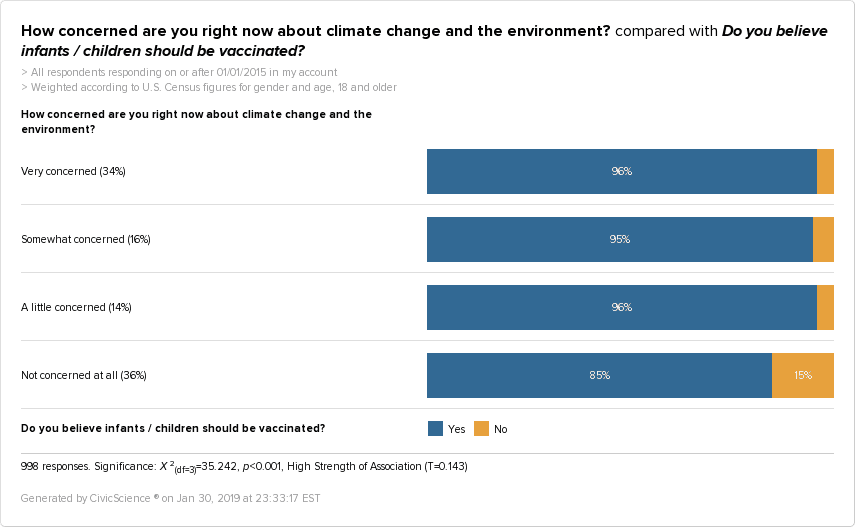
Climate Change — There is a correlation between lack of concern for climate change and childhood vaccine hesitancy. Of those who say they are not at all concerned about climate change and the environment, 15% are not in favor of childhood vaccination. That number stands in stark contrast to those who have some level of concern for climate change.
Looking Ahead
Ultimately, we’re left with a complex picture behind a public health crisis. But however thorny, it’s one that’s not immune (no pun intended) to having its own set of demographics and idiosyncrasies — young adults, high earners, and organic food buyers, to name a few.
While vaccination campaigns have saved the lives of millions worldwide within the past 20 years alone, uncertainty surrounds the future of vaccination rates and further disease outbreak, in the U.S. and abroad. Will the outbreaks serve as a clarion call to change public perception, especially for young adults, or are we sitting on a ticking time bomb?